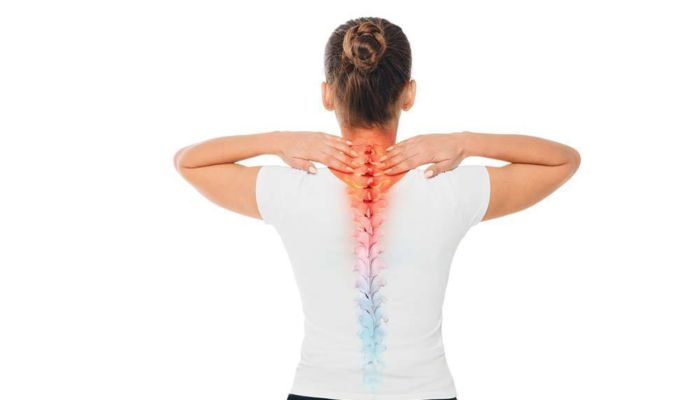
As we age, we can experience age-related health issues, such as back pain. One of the most common age-related problems is degenerative disk disease, which is actually not a disease, but a natural condition in the body that results from age alone. Disk degeneration often occurs comorbidly with sciatica, which is another painful back condition. Read on to learn more about degenerative disk disease and sciatica, what symptoms are like, and what treatments are available.
What Is Degenerative Disk Disease?
A good analogy is to think of the disks (which are located on the spine) like shock absorbers in a car. The function of shock absorbers is to help absorb shock and movement as a vehicle is being driven. Over time, shock absorbers wear down and require replacement, or there’s a bit of a bumpy ride. The disks in your spine have a rubbery consistency, and they too wear out over time. Their function is to absorb the tiny shocks as you walk and perform other tasks. When they wear out, it can be painful. The name associated with the disks wearing out over time is degenerative disk disease. Not everyone who ages will develop degenerative disk disease, even though everyone’s disks do experience wear and tear over time. If you have painful disks in your back, then it’s likely you have degenerative disk disease.
Disks can also rupture from wear, and this is what is known as a herniated disks. A series of herniated disks in the lumbar spine is called sciatica. Sciatica can be caused by disk herniation or from osteoarthritis and is associated with a curvature of the spine because of the location of the herniated disks (low back).
What Causes Degenerative Disk Disease?
Age is the cause of degenerative disk disease, but there are reasons behind it. As we age, our protein and water content changes, which affects the body as a whole - not just the spine. However, the overall effect of this is weaker cartilage. To think about why this is harmful to the spine, we must think about the shape of the spine. The vertebrae in the spine comprise the majority of its construction. In between the vertebrae are the disks, which are constructed mainly of cartilage. Disks are located between each larger portion of the vertebrae, so they are situated in the neck (cervical spine), mid-back (thoracic spine), and the lower back (lumbar vertebrae). The disks are fundamentally made of cartilage, but so are the joints between the vertebrae. The overall effect is the wearing down of the joints and disks over time. If one of the disks cracks or ruptures, then the disk is herniated, which can cause excruciating pain.
Beyond age, there are certain risk factors associated with the development of degenerative disk disease. These include obesity, tobacco usage, trauma (such as a slip or fall), and strenuous physical labor. Sometimes patients notice the problem for the first time soon after a motor vehicle collision or other physically traumatic events. Age remains the most significant risk factor.
What Are the Symptoms of Degenerative Disk Disease?
Your entire spine may have degenerative disks or just a portion of the spine. You may feel sharp constant neck pain, lower back pain, mid-back pain, or a combination of the three. Take careful note of how the pain feels so you can let your healthcare provider know. He or she will ask specific questions about the pain to help diagnose you. Degenerative disk disease pain may feel like:
- Pain that comes and goes
- Improves when you change positions or at night
- Is prevalent when you sit and improves with movement
- Is in your buttocks, upper thighs, or lower back
- Is in your neck
Beyond pain, those with degenerative disk disease may feel numbness or tingling in the arms or legs, which could potentially lead to muscle weakness. This is because disks are very close in proximity to nerve endings in the spine. Because they are not properly absorbing shocks, the nerves are then affected. Low back pain is also known as lumbago, which can irritate the main spinal nerve. Spinal irritation is called radiculopathy. If your degenerative disks have progressed to herniation, sciatica symptoms are slightly different. Pain associated with sciatica often “shoots” down the lower extremities. Pain may be constant and may increase with movement, coughing, or sneezing. Those with severe sciatica may also experience incontinence.
Diagnosing Degenerative Disk Disease
Doctors use a few methods to diagnose degenerative disk disease other than a patient interview. After you tell your physician where the pain is located, he or she will likely perform a physical exam to check for back problems. Your doctor will look for muscle atrophy or muscle wasting, and may also check your muscular strength. You may also be asked to move in specific ways to further pinpoint where your back pain is located. Your doctor may also check your nerves (reflexes) with a hammer, such as during your yearly physical. If you have poor to no reaction, that could indicate a problem with the spinal nerve. You also may be checked to see how your nerves respond to temperature changes.
For diagnostics, X-ray is commonly used, which can also detect osteoarthritis. CT and MRI scans are also options. Your doctor also may order electromyogram (EMG) or nerve conduction velocity (NCV), which can both check your lower extremities for problems. Most commonly, physicians use CT and MRI for degenerative disk disease and EMG and NCV for sciatica.
Treatment of Degenerative Disk Disease
Over-the-counter or prescription-strength nonsteroidal anti-inflammatory drugs (NSAIDs) are common to treat degenerative disk disease and sciatica pain. This condition may also trigger muscle spasms in your legs, so you may need medication for that as well. Physical therapy can help with flexibility in your back and neck, and regular physical therapy can help prevent degenerative disk disease pain. A steroid injection in the epidural area of the back near the spinal cord is also an option for severe pain. In many cases, medications and physical therapy are adequate treatment.
Surgery is also an option if medication and physical therapy are not effective. Stabilization surgery, or spinal fusion, can connect two vertebrae together to help relieve pain. Decompression surgery is also an option to relieve pressure on the nerves.
If degenerative disk disease is comorbid with sciatica, osteoarthritis, or spinal stenosis, the patient may need additional forms of treatment or surgical options. Stem cell therapy is also in the evaluation stages to see if it is an effective degenerative disk disease treatment. If you need more information about degenerative disk disease or sciatica, or wish to be seen by a physician, request an appointment at NewSouth NeuroSpine today. We have specialists in surgical intervention, physical therapy, spinal intervention, and rehabilitation who can help you achieve a better quality of life without pain.