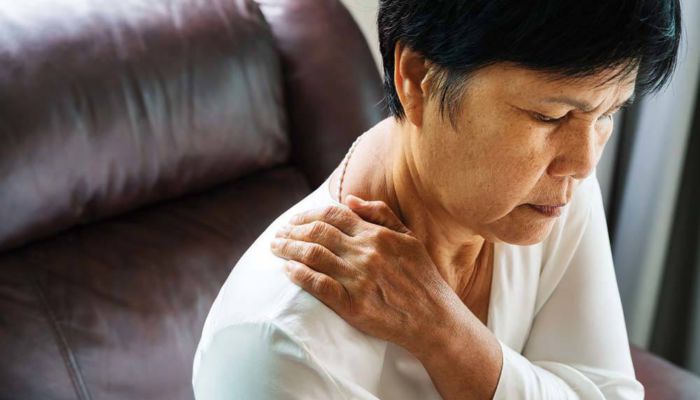
Sometimes the cause of pain in the body is easy to identify. Other times, the cause of symptoms could originate somewhere seemingly unrelated. This is the case with a condition called thoracic outlet syndrome. Pain, tingling, numbness, fatigue, discoloration and even muscular atrophy in the hands and arms can all be caused by pressure on the veins, arteries and nerves that supply blood flow and neurological signals to your arm.
These vessels and nerves all pass through a small area under your collarbone called the thoracic outlet. When pressure from tissues like the scalene muscles of the neck, or bones such as the clavicle and the first rib, compress these vessels and nerves, you may experience a variety of symptoms.
If you are suffering from arm pain, numbness in the hands or swelling in one or both of your hands and arms, there may be good news. Many cases of thoracic outlet syndrome can be treated with physical therapy and symptoms can sometimes be eased by taking over the counter drugs like ibuprofen. Long term use of NSAIDS, such as ibuprofen, is linked with an increased risk of bleeding and conditions of the gastrointestinal tract. These medications are meant for short term use only; if you find yourself reaching for the NSAIDS more and more frequently make an appointment with an NS2 physician today. If the cause of your symptoms can be addressed soon enough, you may even be able to alleviate or eliminate them. If these options do not provide relief, surgery may need to be considered, though this is usually a last resort.
What is Thoracic Outlet Syndrome?
Thoracic outlet syndrome (or TOS) is a name given to a complex series of disorders affecting the nerves and blood vessels of the arm. These vessels and nerves pass to the arm between the first rib and collarbone through the thoracic outlet. Compression on these nerves and blood vessels can cause a host of symptoms, and arises from a variety of different causes.
Skeletal issues, either from congenital defects such as having an extra rib (called a cervical rib) or even bad posture, can cause the thoracic outlet to compress. Muscles such as the scalene muscles which run along the sides of the neck can also put pressure on the thoracic outlet. When skeletal or muscular issues are at play, your symptoms are likely to come on slowly and may slowly get worse over time.
Trauma is sometimes the cause of thoracic outlet syndrome, Whiplash from a car accident, for example, can cause significant damage to the neck and spine. In other cases, symptoms arise from repetitive use such as in throwing sports, bodybuilding or job-related movements. Obesity is sometimes cited as a cause of TOS, as extra pressure is exerted on the tissues of the shoulder. Pregnancy can also be a cause, and in some cases, there is no obvious reason for the onset of symptoms.
Poor posture can also be a cause of TOS. Thoracic Outlet Syndrome can occur on either side of the body, and in some cases, it may affect both arms, especially if your posture or job activities are contributing to your symptoms. For people who work in office environments or who type for long periods of time, the shoulders can roll forward, increasing pressure on the clavicle and compressing the thoracic outlet. No matter the cause, the effect is usually the same—compression on the blood vessels and nerves which supply the arm.
What are Thoracic Outlet Syndrome Symptoms and Signs?
The symptoms of thoracic outlet syndrome can vary and will be related to the kind of pressure in your thoracic outlet. In the cases where nerves are being compressed, tingling, numbness and even muscular atrophy will be present. If the blood vessels passing through your thoracic outlet are being pinched, your arm either becomes very pale or can sometimes swell and turn blue.
Neurogenic thoracic outlet syndrome occurs when the brachial plexus is compressed. This bundle of nerves carries motor and sensory signals from your entire shoulder and arm to and from the spinal cord. Since all sensation from your arm must pass through this point, pressure on the brachial plexus can be related to different conditions throughout your arm and hand. Neurogenic TOS can be a cause for concern if left untreated, as long-term nerve damage can result.
If signals relating to sensation are being interrupted, you may experience numbness or tingling in your hand or arm. Sometimes pain is also felt and can extend up into the shoulder and neck. Other symptoms not directly related to sensation can also occur, such as the wasting away, or atrophy, of muscles. This is sometimes seen in the atrophy of the base of the thumb in a condition called Gilliatt-Sumner hand.
Vascular thoracic outlet syndrome results from pressure on the arteries and veins running under the collar bone are compressed. This type of TOS can take multiple forms, and can even be specific enough to be identified as either venous or arterial depending on which vessels are impacted. Like neurological thoracic venous outlet syndrome, you may experience numbness and tingling in the arms with vascular thoracic outlet syndrome.
In venous thoracic outlet syndrome, the subclavian vein is compressed, causing blood to pool in your arm. This can result in your hand becoming bluish and discolored or you may experience swelling in your arm. The extra pressure from the excess blood will sometimes cause pain as well. Blood clots can also be associated with venous TOS, which can be a serious issue. If your surgeon suspects you may have blood clots as a result of your venous TOS, he may prescribe a course of medication to try to dissolve the blood clot before performing surgery.
In the case of arterial thoracic outlet syndrome, rather than blood pooling in your arm because of a blocked vein, blood flow is restricted before it reaches the arm. Compression of the subclavian artery can cause a weak or non-existent pulse, cold fingers or hands, fatigue in the arm and even a lack of color in your hand and fingers. It is even possible to have a throbbing lump near your collarbone at the thoracic outlet. Arterial TOS can also carry the risk of blood clots if the arterial wall has been damaged.
Some medical professionals list a third type of TOS, but this designation is somewhat contested. “Nonspecific-Type Thoracic Outlet Syndrome” is the term used when chronic pain which worsens with activity is felt in the area of the thoracic outlet, but no obvious cause of the symptoms can be identified.
What is the Treatment for Thoracic Outlet Syndrome?
Treatment options for your thoracic outlet syndrome will differ depending on your symptoms. First, your doctor will perform a physical examination to determine the cause and severity of your TOS. Usually, an X-ray or tests such as nerve conduction studies if neurogenic TOS is suspected, are also used to narrow down the cause of your symptoms. Unless x-rays or other imaging indicate surgical treatment is necessary, treatment of thoracic outlet syndrome usually begins with physical therapy. It is possible you may have to incorporate anti-inflammatory drugs to relieve pressure or clot-dissolving medications if you have vascular thoracic outlet syndrome that has resulted in blood clots.
If your symptoms can be treated with physical therapy, your physical therapist will likely focus on exercises designed to strengthen the muscles of the shoulder and to stretch the chest and shoulders. Improving posture and working on your range of motion are also goals that assist in opening up the thoracic outlet.
For cases where physical therapy or medications are not providing relief, or if your thoracic outlet syndrome is related to a congenital skeletal condition or caused by trauma, surgery may be necessary. There is a risk of complications in any surgery, and the possibility of damage to the brachial plexus means your doctor will likely not recommend surgery unless it is absolutely necessary.
Another reason surgeries are usually avoided for thoracic outlet syndrome is they often involve removing tissue. In some cases, your surgeon may actually have to remove the muscles which are causing the compression of the brachial plexus or blood vessels. Depending on the source of your vascular or nerve compression, you may also need to have a portion of your first rib removed to relieve pressure. This procedure, known as a first rib resection, is sometimes necessary, though it is not recommended for all types of thoracic outlet syndrome. Removing the scalene muscles on the affected side of the neck can also bring relief for some patients.
Is it Possible to Prevent Thoracic Outlet Syndrome?
It may not be possible to completely prevent thoracic outlet syndrome, especially if you have a congenital condition that predisposes you to it. There are, however, several things you can do to lessen your chances of developing symptoms or alleviating them if you have already been diagnosed.
Maintaining good posture is one of the best things you can do to fight thoracic outlet syndrome. Along with the other benefits of good posture, opening the chest and rolling the shoulders back will help alleviate pressure in the thoracic outlet. This can be very hard for people who spend long hours working at computers or in an office environment. Taking frequent breaks and stretching can help ease symptoms, and beginning a program of exercise to strengthen the back, shoulders and neck will help keep you from dropping back into old habits.
For some people, avoiding certain activities that worsen symptoms may be part of the recovery process. If sports or work-related activities have brought on pain, tingling or numbness, you may have to adapt or discontinue those activities. This can be challenging for people whose jobs involve motions and activities that contribute to their symptoms.
Other job or lifestyle-related activities can contribute to thoracic outlet syndrome. Carrying heavy bags can compress your shoulder, adding pressure to the collarbone. If you often carry a heavy bag over one shoulder, you may want to consider switching shoulders or using a bag with two shoulder straps to distribute the weight.
When to Talk to Your Doctor About Thoracic Outlet Syndrome
Many people who suffer from thoracic outlet syndrome experience pain or other symptoms for years before seeking treatment. Since symptoms can come on slowly, and may only appear periodically following certain activities, many cases of thoracic outlet syndrome can go undiagnosed for long periods of time.
If your symptoms are worsening, and particularly if you see signs such as muscle weakness or atrophy or bluish discoloration in your hand, you should talk to your doctor. Symptoms can be relieved without permanent damage in many cases, but prolonged pressure on the nerves and blood vessels leading to your arm can lead to damage. If you are experiencing symptoms such as tingling and numbness in one or both of your hands or arms, or have discoloration, pallor or swelling in one arm request an appointment today at NewSouth NeuroSpine. We can help evaluate your symptoms, and determine if treatment will be necessary to get you on a path to recovery.